Life – or perhaps I should say death – was so much easier in the old days.
As end-of-life researcher Joanne Lynn puts it, life threatening illness would “strike without warning and you get through it or you don’t.”
Effective treatments were few. Doctors would often prescribe “remedies” like bloodletting, purges, enemas, blistering, and “medicines” like mercury, lead, and arsenic that did more harm than good - many positively horrific.
George Washington died after he was treated with blister beetle extract applied to his throat and being drained of about 40 percent of his blood volume.
There were guides like Ars moriendi (The Art of Dying), a popular work originally published at the time of the Black Death, that encouraged acceptance, and told you how to die gracefully, without succumbing to lack of faith, despair, impatience, spiritual pride or avarice.
New and Complicated
Now it’s complicated. You are often having to make decisions. Pick from options like CPR, intubation, a ventilator, feeding tube, dialysis, IV fluids, antibiotics, chemotherapy and more.
Consequently, everyone is being urged to decide and document what they do or don’t want before they get to the end. Part of this push is declaring April National Healthcare Decision Month, and April 16th National Healthcare Decision Day.
Like me, you may have been unaware of this, and I’m sorry I missed it. But I use this as a pretext to write about the important business of end-of-life care – even though it’s spring, and perhaps your thinking new life rather than death.
Doctors, motivated by it being seen as such bad form for their patients to die – and perhaps sometimes by business considerations dare I say it - have tended to be a little overzealous.
“Do everything” has become the default mode.
It has also encouraged people to think they can be kept alive forever – and there is that joke about “Americans are the only people who think death is optional.”
But there’s a downside. Surgeon and author Atul Gawande, in his book Being Mortal, notes, talks about getting on that conveyer belt that he calls ODTAA – the “one damn thing after another.”
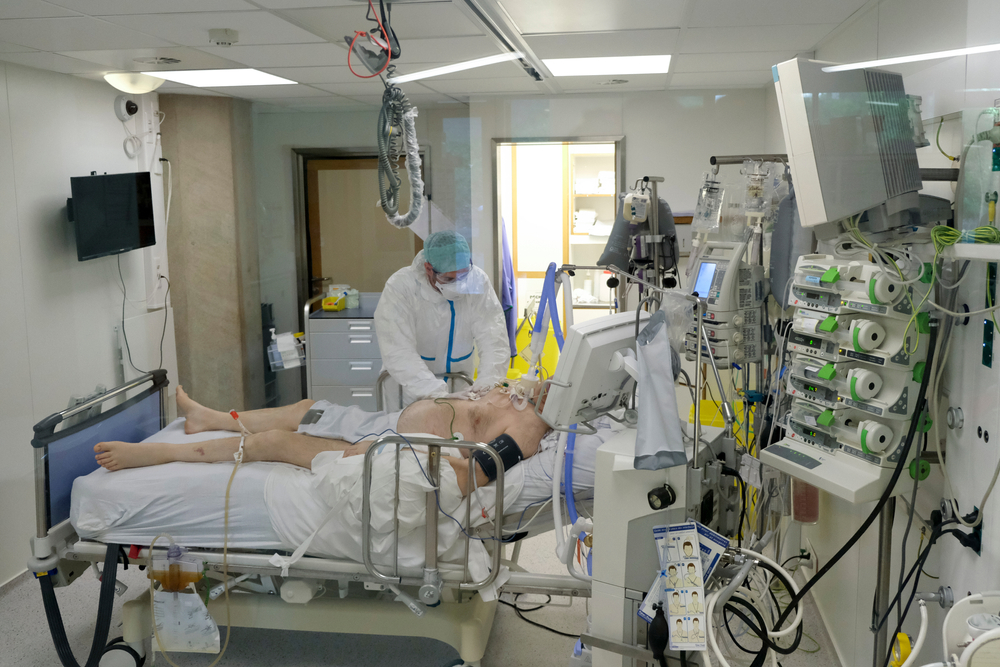
A cascade, where one intervention leads to another and then another. So the end of your life is spent in the ICU on a ventilator, a tube in every orifice, unable to communicate and unable to perform the all-important “dying role” like getting finances in order, saying goodbye’s, resolving personal conflicts etc.
Or maybe you are being hustled into another round of chemo’ that’s only going buy you a few extra days or weeks, but make you sick as a dog. Or are gradually asphyxiating from lung disease like COPD or neurological degeneration like ALS. Or you have pain that cannot be controlled.
There’s that popular quip you hear old farts exchange when one complains “my eyesight’s going, my back hurts, I have to get up all night to pee” and the other retorts “it beats the alternative.”
But there may be times when living – or more exactly protracted dying – may not be better than the alternative.
This is the position of people and organizations like Compassion and Choices who support medical aid in dying where prescribing of a lethal dose of sedative is allowed.
Advice Abounds
There are many sources of information and advice now available to help with end-of-life planning, and there seems to be a lot of interest.
Retired hospice bereavement counselor Gloria Lloyd, and I have been co-organizing an ‘End Of Life Conversations’ group enthusiastically attended by many – admittedly mostly senior citizens who maybe feel the proximity.
Last meeting we discussed the movie and book When My Time Comes by Diane Rehm. Other books about end-of-life care are A Beginners Guide to the End, Knocking on Heaven’s Door, and, as mentioned, Being Mortal.
Amongst organizations, The Conversation Project is very active with a lot of information on their website. Their main push is to get families to “gather round the kitchen table” and share their wishes for the end.
There’s also The End Well Project, The Five Wishes. The Netflix documentary End Game. Or just Googling “help with end-of-life decisions” will lead you to a ton of stuff.
Your doctor should be a good resource - though the stat’s show 8 of 10 people want to talk to their doctor about end-of-life decisions, but fewer than 1 in 10 actually do.
The basics are to create a Living Will, and appoint a Power of Attorney to make decisions if you are incapable. Finding a lawyer who specializes in this stuff is a good move. Also, to make sure your wishes are followed you need to let everyone know what you want.
Death and dying tend to be hidden away in hospitals these days and this natural part of our life cycle has become taboo. I think we need a new Ars moriendi – or at least the attitude of acceptance that goes with it. And advanced planning on how we handle our end-of-life.
This may not be “do everything.”


